Rheumatoid arthritits; symptoms, causes, and treatments.
Rheumatoid arthritits
Rheumatoid arthritis; (RA) is a chronic inflammatory condition, that can harm more than just your joints. Many different body systems can be damaged by it.
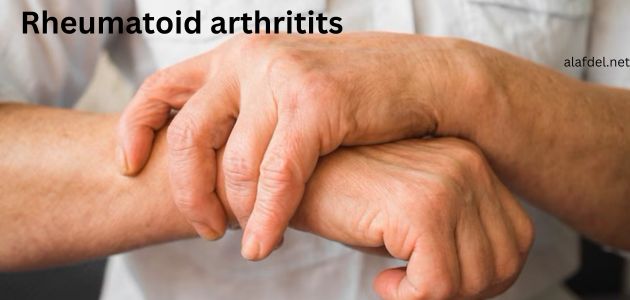
Rheumatoid arthritis (RA) is an autoimmune disorder, where the immune system suddenly attacks the body’s own tissues, causing pain and inflammation. The heart, lungs, and eyes are just a few of the organs that RA may affect, leading to complications like heart disease, lung problems, vision loss, and anemia, which happens when the body lacks enough red blood cells. This condition can cause fatigue and weakness. keep reading in this assay to learn more about rheumatoid arthritis.
Rheumatoid arthritis symptoms

Smaller joints, particularly those connecting your fingers and toes to your hands and feet, are typically the first sign of being impacted by early rheumatoid arthritis. As the disease develops, the wrists, knees, ankles, elbows, hips, and shoulders frequently start showing symptoms.
Basic symptoms include:
- pain.
- swelling joints.
- delicateness.
- rigidity, which is more evident in the morning.
- Fatigue is another symptom of RA inflammation.
- loss of appetite.
- weakness
- Extreme fatigue and a deficiency in energy can result from the pain and discomfort, which can make it hard to go to sleep.
Rheumatoid arthritis causes
There is no main cause for rheumatoid arthritis (RA). Factors like the following could be involved:
- Age: You can develop RA at any age, but between the ages of 40 and 60, it is most common.
- Gender: Women are more likely than men to suffer from RA.
- Genetics: HLA class II genotypes are a group of genes that are associated with an increased risk of developing RA in people. People with these genes may be more susceptible to developing RA if they are obese or exposed to environmental risks like smoking.
- History of live births: It’s possible that those with ovaries who have never given birth have a higher risk of having RA than those who have.
- Smoking: Smokers are more likely to get RA.
- Obesity: extra weight increase the possibility of getting RA.
Read also obesity damage
How is rheumatoid arthritis diagnosed?
Your doctor will talk about your symptoms, medical background, and risk factors. They will do a full physical examination, checking swelling, discomfort, and range of motion in your joints. They will probably also want blood testing to confirm the clinincal examination.
A rheumatologist may use a variety of blood tests to help them decide whether you have RA. These tests consist of:
- Rheumatoid Factor (RF) Test: Autoimmune disorders, particularly RA, are associated with high levels of rheumatoid factor.
- Anticitrullinated peptide antibody Test (anti-CCP): The anti-CCP test often results in RA before the RF test and is more RA-specific than the blood test for RF.
- Erythrocyte sedimentation rate (ESR): The ESR test assists in determining the degree to which inflammation is present in your body.
- C-reactive protein (CRP) Test: Anywhere in your body, a serious illness or significant inflammation might cause your liver to produce C-reactive protein. This inflammatory marker has been linked to high levels of RA.
Other imaging tests can identify damage brought on by the disease in addition to blood tests for rheumatoid arthritis:
- X-rays: X-rays can only find more severe RA. The scans don’t discover early soft tissue inflammation. A series of X-rays taken over a few months or years can be used to detect the development of RA.
- Magnetic Resonance Imaging (MRI): MRIs can identify RA-related inflammation much earlier than an X-ray. However, They aren’t frequently used to identify the disease.
Your doctor will examine these images to determine how much the bones, tendons, and cartilage have been affected. Determining the ideal treatment plan with the help of this evaluation. Since there is no one test to diagnose RA, a diagnosis must be confirmed over time. Consult a doctor as soon as you suspect you may have RA.
Rheumatoid arthritis vs. osteoarthritis
Osteoarthritis (OA) and RA are two major forms of arthritis. They are quite different disorders, but both result in discomfort and damage to the joints.
RA is an autoimmune disorder. It occurs when your immune system doesn’t function properly. When you’re in good health, your immune system fights against foreign invaders like viruses and bacteria. Your immune system attacks your joints when you have RA because it “sees” them as enemies.
OA is not an autoimmune disease. You develop it when the cartilage (spongy tissue) between your joints decreases, which frequently happens as a result of normal wear and pressure. The bones on either side of the cartilage begin to change and become tender as a result.
Although OA can affect any joint, it frequently occurs in those that have been damaged or repeatedly used. Consider your thumbs, big toes, back, neck, knees, and hips.Problems with joints might develop throughout your body as a result of RA. The condition is most prevalent in your hands’ and feet’s tiny joints. It also affects the ankles, knees, shoulders, and elbows. RA typically leaves your back alone, in contrast to OA.
These might be the most significant distinctions between rheumatoid arthritis (RA) and osteoarthritis (OA). However, there are numerous others that can assist medical professionals in identifying the types you have and determining the best course of action.
Rheumatoid arthritis treatment
we should manage rheumatoid arthritis to decrease inflammation, reduce discomfort, and prevent organ and joint damage.
Medications for rheumatoid arthritis treatment
To treat your RA, your doctor might recommend a number of different medications. These medicines consist of:
- Disease-modifying anti-rheumatic drugs (DMARDs): DMARDs can help decrease the symptoms of rheumatid arthritis and slow down its progression.
- Biological treatments: These medications are injected, and they function in coupled with DMARDs.
- Corticosteroids: Short-term prescriptions of corticosteroids are sometimes given to treat inflammation.
- Pain management medication: Prescription medications such as acetaminophen, nonsteroidal anti-inflammatory drugs (NSAIDs), opioids, or muscle relaxers can be used to reduce the pain of an RA flare-up.
- JAK inhibitors: JAK inhibitors are a newer kind of DMARD that are sometimes used to mange severe cases of rheumatoid arthritis.
Supportive therapy for rheumatoid arthritis treatment
- Physical therapy.
- Complementary therapies: such as massage therapy.
- Occupational therapy.
- Surgeries: RA sometimes requires surgical treatment to fix damaged joints.
Home treatments for rheumatoid arthritis
- Eat a nutritious diet.
- Try supplements: according to some studies, omega-3 fish oil and turmeric can decrese rheumatoid arthritis pain. Always consult your doctor before starting any supplementation.
- Maintain an active lifestyle.
- Take time for rest.
- Use cold to calm inflammation.
- Use topical medications: Painkillers for your joints and muscles include creams, gels, and stick-on patches.
- Heating pads and warm baths can both relieve stiff joints.
Know about best 10 foods for diabetics
Although there is no known treatment for RA, early detection can help you manage the disease, keep you active, and enhance your quality of life.
We’ve covered a lot of information regarding the causes, symptoms, diagnosis, and treatment of rheumatoid arthritis in this article. After being diagnosed with rheumatoid arthritis, you are able to maintain a healthy, active life, even if it may be a lifelong condition. If you take the correct drugs, your symptoms can even be completely under control. Maintaining your level of activity and according to your doctor’s advised treatment plan will provide you the best results and remission chances.

Comments are closed.